- MENU
- HOME
- SEARCH
- WORLD
- MAIN
- AFRICA
- ASIA
- BALKANS
- EUROPE
- LATIN AMERICA
- MIDDLE EAST
- United Kingdom
- United States
- Argentina
- Australia
- Austria
- Benelux
- Brazil
- Canada
- China
- France
- Germany
- Greece
- Hungary
- India
- Indonesia
- Ireland
- Israel
- Italy
- Japan
- Korea
- Mexico
- New Zealand
- Pakistan
- Philippines
- Poland
- Russia
- South Africa
- Spain
- Taiwan
- Turkey
- USA
- BUSINESS
- WEALTH
- STOCKS
- TECH
- HEALTH
- LIFESTYLE
- ENTERTAINMENT
- SPORTS
- RSS
- iHaveNet.com
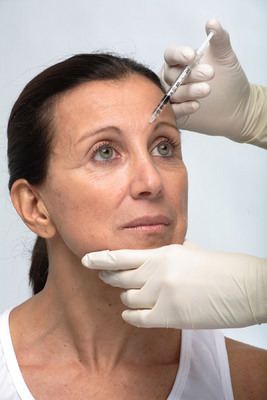
Whether Botox is used for cosmetic or medical purposes, its effects are temporary, so repeated injections are necessary
At one time, most of us knew about botulinum toxin mainly as the source of deadly botulism food poisoning. Produced by the bacterium Clostridium botulinum, the toxin is one of the most lethal substances on earth. Ingested, it can paralyze muscles throughout the body, including those that control breathing. Yet on a smaller scale, the same mechanism can do a body good. Injected into muscle tissue, for example, botulinum toxin can ease debilitating spasms and pain.
The Many Uses of Botox
Today, most of us are familiar with botulinum toxin as Botox, the popular cosmetic treatment approved in 2002 to minimize the appearance of glabellar lines -- vertical furrows between the eyebrows that become more pronounced as we age. By preventing muscle contractions that cause facial lines, Botox smooths the skin and makes it look younger. It's now widely used to treat a range of facial wrinkles, including those that appear on the neck (turkey neck), at the corners of the eyes (crow's feet), and across the forehead.
Botox gets the headlines these days as a wrinkle reducer, but it has a longer history as a medical therapy. In the late 1950s, researchers showed that injecting tiny amounts of botulinum toxin relaxed overactive muscles by blocking the release of acetylcholine, a neurochemical essential for muscle contraction.
In 1989, Botox was approved for the treatment of strabismus (misaligned eyes) and blepharospasm (abnormal squinting and eyelid twitching). Since then, it's been approved for the treatment of cervical dystonia (muscle spasm affecting the neck and shoulders) and hyperhidrosis (severe sweating). Myobloc, which is made from botulinum toxin strain type B (Botox is made from the type A strain), is also approved for the treatment of cervical dystonia. Dysport (another form of botulinum toxin type A) came on the market in 2009 and is approved for both cervical dystonia and glabellar lines.
Botox and its cousins have the official go-ahead for just a few medical indications, but once a drug is approved, it can be prescribed at a clinician's discretion. So the toxin is now being used for a growing list of conditions. Many of these uses make sense given the toxin's effect on muscle action, but some experts are concerned about the lack of studies proving safety and effectiveness.
Before considering a botulinum toxin injection, you should learn about the proven (and often less invasive and less expensive) alternatives. A qualified physician is unlikely to suggest botulinum toxin unless the alternatives have failed, or studies have shown it's the best (or only) option. Keep in mind that unapproved treatments may not be covered by insurance.
Approved Uses of Botox
Strabismus (misaligned eyes)
Blepharospasm (eyelid twitching)
Cervical dystonia (neck spasm and pain)
Hyperhidrosis (excessive sweating)
Unapproved, Off-Label Uses of Botox
Focal dystonias
Cerebral palsy
Tremor
Hypertonia (abnormal increase in muscle tension and reduced ability of a muscle to stretch)
Post-stroke spasticity
Drooling
Excessive salivation
Rhinitis (runny nose)
Tension headache
Migraine headache
Ringing in the ears (tinnitus)
Facial tics
Bruxism (teeth grinding)
Severe jaw pain
Temporomandibular joint syndrome
Trigeminal neuralgia (intense facial pain)
Dysphonia (difficulty producing sounds)
Raynaud's phenomenon
Achalasia (difficulty swallowing)
Stuttering
Tourette's syndrome tics
Piriformis syndrome (sciatic nerve compression in the buttocks)
Facial scars
Anal fissure
Constipation
Pelvic pain
Low back pain
Incontinence
Overactive bladder
Hair loss
Phantom limb pain
Tennis elbow
Whether botulinum toxin is used for cosmetic or medical purposes, its effects are temporary, so repeated injections are part of the therapy. The dose depends, among other things, on your weight, the condition being treated, the preparation used, and the amount of muscle into which it's injected. With repeat injections, muscles may atrophy and lose some function, an effect that's reversed when the injections stop.
Some patients receiving botulinum toxin in large doses for medical conditions have become resistant to the drug, that is, they've developed antibodies that hamper its activity. Resistance may be minimized by giving the smallest effective dose and spacing injections further apart. - Harvard Women's Health Watch
Medical Applications of Botox
It's a good choice for dystonias. Dystonia is a neurological disorder characterized by chronic, involuntary muscle contractions resulting in uncontrollable movements or postures. Focal dystonia is any dystonia limited to a specific group of muscles, for example, cervical dystonia, which involves the muscles of the neck and shoulders, or spasmodic dysphonia, which involves the vocal cords.
Toxin injections have shown beneficial effects on many focal dystonias that do not respond to physical therapy, medications, and surgery. Possible side effects include muscle weakness, flulike symptoms, and dry mouth.
Focal dystonias treated by botulinum toxin:
1. Cervical dystonia (CD): Abnormal, painful positions of the head, neck, and shoulders.
2. Blepharospasm: Involuntary blinking or squinting.
3. Writer's cramp, musician's cramp: Limited finger movement, impairing ability to write or play a musical instrument. In golfers, it can cause trouble putting, called "the yips." Several small trials have found that toxin injections can alleviate hand cramping; to avoid side effects, find a clinician with experience and skill injecting the toxin. Other medications have shown few benefits; surgery is not effective.
4. Spasmodic dysphonia (SD): Spasm of the vocal cords. Disrupts speech and affects voice quality, producing a "strangled-sounding" or (less commonly) breathy voice. The toxin seems to be more effective for SD characterized by a strangled-sounding voice. There are no effective alternative therapies for SD.
5. Easing anal fissure. An anal fissure is a tear in the lining of the anal canal, usually caused by a strained bowel movement or the passage of a hard stool. It causes bleeding and severe pain, and it can trigger a spasm in the underlying sphincter muscle that prevents the fissure from healing. Surgery is the standard treatment, but it causes incontinence in up to 30 percent of patients. Nitroglycerin and calcium-channel blockers may help, but they cause headache in many patients.
Botulinum toxin injection has been used to treat anal fissures since the mid-1990s, and numerous studies have confirmed its effectiveness. According to a report in
Botulinum toxin is more effective overall than topical nitroglycerin, but patients who don't respond to one of these treatments often respond to the other. Because the injections are invasive, it's probably best to try nitroglycerin first. If you need the toxin, insurance usually covers the cost.
6. Myofascial pelvic pain syndrome. Myofascial pelvic pain syndrome (MPPS) is a chronic pain disorder involving muscle contractions and spasms in pelvic floor muscles with unusually tender areas, called trigger points. Symptoms include aching, heaviness, or burning in the vagina, vulva, rectum, or bladder, sometimes extending to the thighs, lower abdomen, or buttocks. Overactive bladder, constipation, and painful intercourse are often part of the picture. The underlying cause is unknown but probably involves a combination of factors. Treatments include painkillers, antidepressants (at doses that reduce pain), psychotherapy, meditation, physical therapy to stretch and strengthen pelvic floor tissues, and anesthetic injections into trigger points.
Botulinum toxin injections are an option for women who get no relief from physical therapy or anesthetic injections. The evidence so far is sparse but promising. A pilot study involving 12 women given Botox injections in the pelvic floor found some pain reduction. In a randomized controlled trial involving 60 women with chronic pelvic pain, Botox was more effective than a placebo in reducing pelvic-floor muscle pressure and some types of pain.
7. Botox for headache? Probably not. Researchers began to study Botox as a treatment for headaches after migraine patients getting cosmetic injections reported having fewer headaches. Scientists speculated that the toxin suppresses not only muscle contractions but also pain signals. But now, data suggest that the toxin isn't much better than a placebo in treating most headaches.
Based on a review of 11 randomized controlled trials, researchers reported in the journal Neurology (2008) that the toxin was "probably ineffective" in treating episodic migraine and chronic tension headache. As a result, the
Other Uses of Botox
There's reasonably good evidence that botulinum toxin is safe and helpful for several other medical conditions, such as hemifacial spasm (chronic facial muscle contraction), achalasia (a rare esophageal disorder that makes it difficult to swallow food), axillary hyperhidrosis (excessive sweating from the armpits), palmar hyperhidrosis (excessive sweating of the palms), essential hand tremor, and spasticity from conditions such as stroke and multiple sclerosis.
Toxin injections are no cure-all. As noted above, reports have underscored their limits as a headache treatment. And although the
Black-Box Warning and Other Safety Issues
In
The
Finally, if you're considering botulinum toxin injections for any reason, cosmetic or medical, the standard caveats apply: Look for a licensed, board-certified physician who has extensive experience with botulinum toxin and its potential side effects. Don't be afraid to ask questions. Request permission to speak to a patient the clinician has treated. And before treatment, be sure to tell your physician about any prescription or over-the-counter medications you're taking, as well as anything you're allergic to and any medical problems you might have.
AGING | ALTERNATIVE | AILMENTS | DRUGS | FITNESS | GENETICS | CHILDREN'S | MEN'S | WOMEN'S
© Tribune Media Services