- MENU
- HOME
- SEARCH
- WORLD
- MAIN
- AFRICA
- ASIA
- BALKANS
- EUROPE
- LATIN AMERICA
- MIDDLE EAST
- United Kingdom
- United States
- Argentina
- Australia
- Austria
- Benelux
- Brazil
- Canada
- China
- France
- Germany
- Greece
- Hungary
- India
- Indonesia
- Ireland
- Israel
- Italy
- Japan
- Korea
- Mexico
- New Zealand
- Pakistan
- Philippines
- Poland
- Russia
- South Africa
- Spain
- Taiwan
- Turkey
- USA
- BUSINESS
- WEALTH
- STOCKS
- TECH
- HEALTH
- LIFESTYLE
- ENTERTAINMENT
- SPORTS
- RSS
- iHaveNet.com: Health
Harvard Health Letters
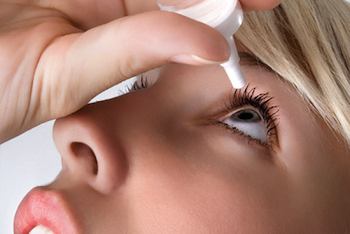
Eye drops that get the red out do so by constricting blood vessels in the eye. These vessels can become insensitive if drops are applied too often.
Harvard Health Letters
We notice tears when we cry and when others do. Psychologists theorize that weeping is an "attachment behavior" designed to get others to help us -- you might say that tears are a cry for help. There's an old theory that sobbing may help fend off infections, the notion being that some of the overflow drains into the nose through the tiny ducts that connects the inside corners of the eyes to the nose. In the nose, tears moisten nasal mucous membranes so they're more effective at corralling bacteria and viruses.
But if our eyes are healthy, we're actually producing tears all the time and not noticing it very much, if at all. We need a thin layer of tears to lubricate, protect, and nourish the fronts of our eyes. That "tear film," as ophthalmologists call it, isn't just salty water but a complex mixture of substances produced and maintained by several glands and structures in and around the eyes. If the tear film degrades, we experience dry eyes. The symptoms are familiar to many of us: irritation, scratchiness, a burning sensation. Sometimes vision is affected, getting blurry off and on.
Mild cases -- and many are -- can be treated rather easily with any of over a dozen different over-the-counter products. In a change from the past, dry eyes are now seen as having an inflammatory component, not just a loss of moisture. To combat the inflammation, some ophthalmologists prescribe drops that contain a very small amount of cyclosporine if the over-the-counter products don't work. Cyclosporine is a drug that organ transplant recipients take to suppress the immune system so the organ is less likely to be rejected.
A FATTY OUTER LAYER
Traditionally, the tear film has been described as having three separate layers: an inner, mucous layer created by secretions from cells in the conjunctiva, the clear membranes that cover the eye and the inside of the eyelids; a middle, watery layer produced by the lacrimal glands; and a thin outer layer of fat molecules produced by the meibomian (pronounced my-BOW-me-an) glands located inside the eyelid.
A newer, more nuanced characterization of tear film blurs the lines between the layers and divides it roughly into two parts: an inner layer of fluid that is more dense with mucus closer to the eye surface, and the outer layer of fat molecules. Growth factors, infection-fighting cytokines, and other substances float around in the aqueous inner layer. The fatty outer layer is important because it seals in and prevents evaporation of the watery layer behind it.
When intact, tear film serves multiple purposes: it's a physical barrier, a defender against infection, a remover of debris, a moisturizer. Light must pass through it to reach your eyes, so the film needs to be smooth and regular or vision will be distorted.
Dr. Jason S. Rothman, a dry-eye specialist at
OLDER AND DRIER
Dry eyes used to be thought of as a simple problem of not enough tear production, too much tear evaporation, or some combination of both. Dry eyes may still begin that way, but now the thinking is that localized inflammatory processes get started as the tear film loses moisture.
Air conditioning during the summer -- and indoor heat during the winter even more so -- makes the air inside our homes bone-dry, so water in tear film and other bodily surfaces evaporates easily. Blinking levels out and replenishes the fatty outer layer of the tear film, and normally we blink every 10 seconds or so. Activities that decrease that rate -- watching television, working at a computer, driving a car -- can cause dry eyes because they slow down the blink rate.
Age is a factor: the older orb tends to be a drier one because the lacrimal and other glands become less productive. And with age, lower eyelids may sag, so they don't form a good seal over the eye. In general, women are more prone than men to have dry-eye problems because they have lower levels of androgens, the male sex hormones, and the meibomian glands are, in part, activated by androgens landing on receptors there.
Autoimmune diseases, conditions in which the immune system turns on the body instead of throwing itself at invading infections as it is supposed to, can affect tear film ingredients and cause dry eyes. Lupus and rheumatoid arthritis are two such diseases. And tearless, dry eyes are one of the signature symptoms of Sjogren's syndrome, an autoimmune disorder that affects the lacrimal, salivary, and other glands that produce moisture.
Inflammation of eyelids, or blepharitis, affects the production of the meibomian glands, so the tear film loses its protective outer fatty layer and evaporates more easily. Blepharitis occurs frequently in people with allergies and with skin conditions such as rosacea and seborrheic dermatitis.
Dry eyes are also a side effect of some commonly used medications, including antihistamines, beta blockers, and the selective serotonin reuptake inhibitor (SSRI) antidepressants, such as citalopram (Celexa) and fluoxetine (Prozac). Some over-the-counter eye drops contain benzalkonium chloride, a preservative that can dry out eyes and have other side effects. Benzalkonium chloride is also an ingredient in many of the prescription drops for glaucoma.
Dry eyes are a common side effect of LASIK to correct nearsightedness and farsightedness, although it's usually temporary. Contact lenses reside within the tear film, and dry eyes are one of the main reasons some people can't wear contact lenses or can only do so on a limited basis. Sometimes switching the contact lens solution or trying lenses made out of a different material can help.
Conjunctivitis, inflammation of the conjunctiva, is also known as pink eye. Most conjunctivitis is viral, and there isn't any treatment other than waiting the infection out, but bacterial conjunctivitis can be treated with antibiotic drops. Many allergies affect the eyes, although the main complaint is usually itchiness or watery eyes, not dryness.
GETTING THE RED OUT COULD BE INVITING TROUBLE
Visine and other drops that "get the red out" do so by constricting blood vessels in the eye. They contain a vasoconstrictive chemical called tetrahydrozoline. Blood vessels become insensitive to the effect of tetrahydrozoline if it's applied too often, so more drops need to be applied to have the same effect.
It's fine to use Visine on occasion, but if you need it all the time, you should see an ophthalmologist. Not all Visine products contain tetrahydrozoline, and the artificial tear products sold under the famous brand name are fine to use on a long-term basis.
DIAGNOSING THE PROBLEM
There's no specific test to diagnose dry eyes. Most ophthalmologists will examine the eyes with a slit lamp, the device with the chin rest and bright light that the doctor uses to peer into our eyes. Eye drops with special stains can be used to evaluate the health of the eye surface and gauge the stability of the tear film. The Schirmer test uses small strips of filter paper to quantify the tear production for each eye, although the results may be variable.
Frequently, though, the eye exam and test results are secondary in the diagnostic workup, especially if the problem is mild. Symptoms and the patient's history are often the key pieces of information in arriving at a diagnosis.
TREATING DRY EYES
If the source of the problem is dry air, using a humidifier can make a big difference. Limiting screen time (TV, computer monitors), which is bad for many body parts, not just those we see with, can also help.
But the first-line treatment for most people with dry eyes remains an over-the-counter topical treatment of some kind, typically drops. These products are referred to as artificial tears, which are a bit misleading because they lack the growth factors, cytokines, and other biologically active ingredients of the real thing. Artificial tears usually contain some cellulose to make them thick and viscous.
Substances like polyethylene glycol or polyvinyl alcohol are added so they spread evenly, and most brands have a preservative of some kind. The starting dose is usually a drop in each eye four times a day. They can be used more frequently, but because the preservatives can be irritating if used more than four times a day, some people are advised to switch to drops that are packaged as single doses so a preservative isn't necessary.
Single-dose drops don't have preservatives but are more expensive. Artificial tears also come as gels and ointments. They're thicker than the drops and can make it hard to see, so people often apply them only at bedtime.
Prescription cyclosporine drops are usually used after patients have tried the over-the-counter products. Findings reported in the Archives of Ophthalmology in 2008 showed that about 70 percent of the 191 dry-eye patients in the study who hadn't had good results with artificial tears responded well to cyclosporine drops.
Despite this and other supportive results, some ophthalmologists remain skeptical about cyclosporine drops because they haven't seen such good results in their own patients. Cyclosporine drops take some time to work -- between six and eight weeks in most cases. Price is a drawback: sold under the brand name Restasis, they cost about
Results from a
Other researchers have reported positive results for omega-3 eye drops in mice. On the could-help-can't-hurt principle, some ophthalmologists instruct their dry-eye patients to increase their omega-3 intake either by eating more fish (salmon is the best source) or by taking an omega-3 supplement.
OTHER TOOLS IN THE KIT
Other kinds of drops can be used. Corticosteroid drops have a strong anti-inflammatory effect but must be used very sparingly because continued use can cause cataracts and glaucoma. Some patients who haven't responded well to other remedies do well with autologous serum tears: drops made with sterile salt water and the patient's serum, the clear liquid that is left after blood has clotted.
Punctal occlusion is another choice. The openings of ducts in the eyelids that drain fluid away from the eyes are plugged, so the tears can accumulate and last longer. The plugs can be temporary (made of a dissolvable substance like collagen) or permanent (made of silicone).
Some people try "moisture chambers" that fit on regular glasses and create a seal so moisture from the eyes can't escape. Swim goggles might have the same effect; few of us want to walk around wearing swim goggles, although wearing them at night might not be so bad.
Warm compresses can help if your dry-eye problems are caused by blepharitis because the warmth loosens up the oils in the meibomian glands. Make a homemade compress by filling up a sock with uncooked dry rice and briefly microwaving it. - Harvard Health Letter
Available at Amazon.com:
Last Child in the Woods: Saving Our Children From Nature-Deficit Disorder
Copyright ©. Harvard Health Letters
AGING | ALTERNATIVE | AILMENTS | DRUGS | FITNESS | GENETICS | CHILDREN'S | MEN'S | WOMEN'S
Health - When Eyes Get Dry, And What You Can Try